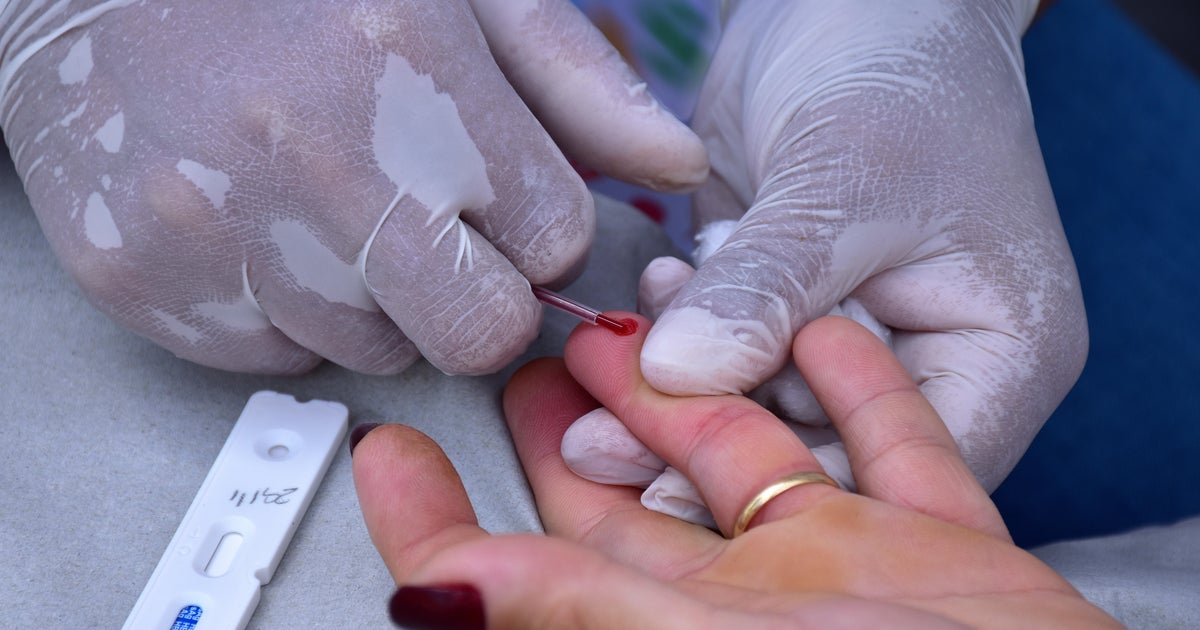
Syphilis is back on the rise across the United States after being nearly eliminated in the late 1990s and early 2000s. But in the Navajo Nation, a solution to curbing the now national epidemic is emerging.
The sexually transmitted infection can lead to serious health problems if left untreated.
Syphilis cases skyrocketed in the U.S. as the Centers for Disease Control and Prevention’s STD prevention budget dropped, data shows. In 2003, the budget was around $169 million and there were about 34,000 cases in the U.S. In 2023, the budget was roughly $80 million and there were about 209,000 cases nationwide.
On Tuesday, the Trump administration began layoffs across multiple federal health agencies including the CDC. While it’s unclear exactly how the cuts will impact STD programs, the CDC’s National Center for HIV, Viral Hepatitis, STD, and Tuberculosis Prevention is affected, in addition to programs for reproductive health, maternal and child health, and HIV.
Grace Manthey
Rates of congenital syphilis, when babies get the infection from their mothers during pregnancy, have increased 10-fold nationally in the last decade, according to CDC data, and the rate for indigenous babies is 8-times higher than those born to White mothers. Congenital syphilis may cause stillbirth, miscarriages, vision or hearing loss, intellectual disability and more.
Most of these cases could be prevented with early testing and treatment during pregnancy.
Health officials in the vast Indian reservations of the Southwest are fighting sexually transmitted infections with a unique program that meets patients where they are to provide treatment.
“The scope of all of this is to ensure that they get treated right away,” public health nurse Melissa Wyaco told CBS News. “We thought that congenital syphilis was eradicated, but it wasn’t.”
Grace Manthey
Faced with a patient population with high rates of poverty, limited transportation and spread across three states, Wyaco’s team hits the road to test patients at food pantries, jails, alcohol treatment centers, churches and motel rooms.
“These are folks who have no home. They’re folks who have no income. They’re just surviving day to day,” said Dr. Jon Iralu, who started his career with the Indian Health Service at the height of the AIDS epidemic and has been fighting infectious diseases in the area ever since.
“It’s all about testing and immediate treatment,” Iralu said. “You have a person right there — you might not see them again.”
He said they’ve seen a greater than 20% drop in cases in some areas.
“If we had done this 10 years ago, before the COVID pandemic, people would have been afraid. People are used to these sort of public health interventions and a little more open,” he said. “I think in some ways, the pandemic was part of the problem, but it’s also part of the solution.”
Those leading the fight are convinced the program, focused on bringing treatments where and when they’re needed most, can be replicated to help patients across the U.S.
“We’re the first ones in the United States to put something like this in place. We’ve put the foundation in place for others to follow,” Wyaco said.